The progression to periodontitis
Periodontitis occurs when anaerobic bacteria in the periodontal pockets causes inflammation, destroying tissue in the periodontium. As a result, the pocket increases in depth and alveolar bone is lost.1,2
Periodontal disease progression can be thought of as a cascade of events2-4
-
1 BACTERIA GROWS
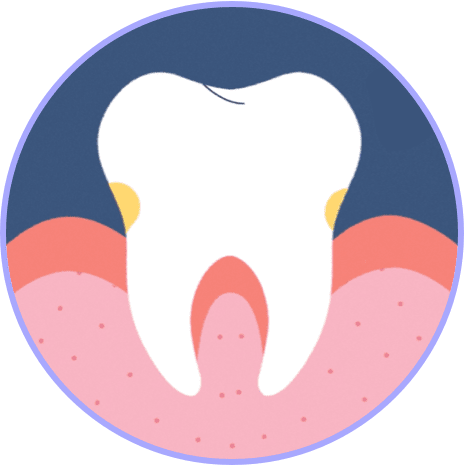
As bacterial infection grows, gum tissue becomes red, swollen, and sometimes bleeds. Pockets form that can become further infected.
-
2 POCKETS DEEPEN
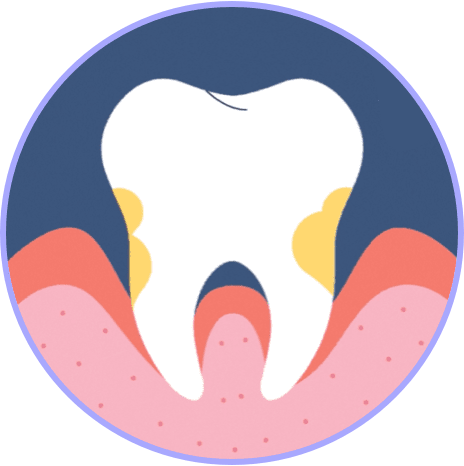
This leads to an inflammatory response, which is primarily responsible for periodontal tissue damage.
-
3 INFECTION SPREADS
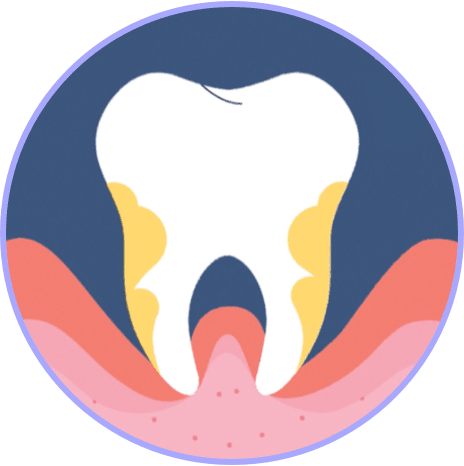
Infection spreads around the tooth. Bone, gums, and connective tissue deteriorates, ultimately leading to tooth loss.
How periodontitis differs from gingivitis
Both conditions are characterized by pocketing and bleeding on probing, but periodontitis is considered more severe for a range of reasons:
-

It’s caused by a combination of factors
Bacterial infection isn’t thought to cause periodontal disease by itself; a person’s immune response may also be a contributing factor. There are differences in the susceptibility of each person that affect the expression of episodic periodontal disease.2
-
It’s associated with systemic diseases and conditions
Inflammation from periodontitis may cause or worsen other inflammatory diseases. Pathogens can also enter the bloodstream through ulcerations caused by the destruction of connective tissue.5 As a result, periodontitis is associated with systemic diseases such as heart disease, stroke, diabetes, rheumatoid arthritis, cancer, respiratory disease (pneumonia, COPD), and the delivery of premature, low-birth-weight babies.6
-

It can result in tooth loss
Progression to periodontitis signifies irreversible bone loss and greater pocket depth due to the person’s immune response, eventually resulting in tooth loss.2
Did you know?
Periodontitis is the #1 cause of adult tooth loss in the united states7


If not caught early and properly controlled, periodontitis can be a chronic, lifelong disease8
Managing periodontal disease from the first sign of infection is a key treatment goal.9
To prevent bone and tooth loss, periodontitis needs to be diagnosed and treated at the earliest stages.5,9 By the time pocket depth is greater than 5 mm, the infection has extended to the middle third of the root or beyond, increasing the chances of tooth loss.10
There’s more than oral health in jeopardy when a patient lives with a chronic oral infection like periodontal disease.6 This may increase a patient's risk of multiple systemic conditions, including cardiovascular disease.5
Have support on hand for your patient conversations
Use the MyPerioHealth assessment tool to help guide your oral health discussions with patients in the chair.
LEARN ABOUT: The unpredictability of periodontitis
Stay in touch
Sign up to receive emails from Back to Basics
REFERENCES: 1. Kornman KS. The pathogenesis of periodontitis. In: Wilson TG Jr, Kornman KS, eds. Fundamentals of Periodontics. 2nd ed. Quintessence Publishing Co, Inc.; 2003:3-12. 2. Kinane DF, Stathopoulou PG, Papapanou PN. Periodontal diseases. Nat Rev Dis Primers. 2017;3:17038. 3. Gum disease information. American Academy of Periodontology. Accessed March 29, 2022. https://www.perio.org/for-patients/gum-disease-information/ 4. Genco RJ. Clinical innovations in managing inflammation and periodontal diseases: the workshop on inflammation and periodontal diseases. J Periodontol. 2008;79(8 Suppl):1609-1611. 5. Tonetti MS, Greenwell H, Kornman KS. Staging and grading of periodontitis: Framework and proposal of a new classification and case definition. J Periodontol. 2018;89(Suppl 1):S159-S172. 6. Cullinan MP, Ford PJ, Seymour GJ. Periodontal disease and systemic health: current status. Aust Dent J. 2009;59(1 Suppl):S62-S69. 7. National Institutes of Health. Periodontal (Gum) Disease. Reviewed August 2021. Accessed March 29, 2022. https://www.nidcr.nih.gov/research/data-statistics/periodontal-disease 8. Shaddox LM, Walker CB. Treating chronic periodontitis: current status, challenges, and future directions. Clin Cosmet Investig Dent. 2010:2:79-91. 9. Lang NP, Bartold PM. Periodontal health. J Periodontol. 2018;89(Suppl 1):S9-S16. 10. Staging and Grading Periodontitis. The American Academy of Periodontology. Accessed April 7, 2022. https://sites.perio.org/wp-content/uploads/2019/08/Staging-and-Grading-Periodontitis.pdf